Treatment of Eczema/dermatitis at community pharmacy
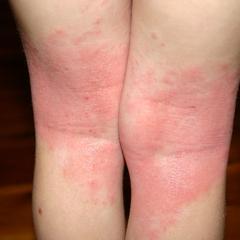 |
| Dermatitis on legs |
Significance of questions and answers
Age/distribution
The distribution of the rash tends to vary with age. In infants, it is usually present around the nappy area, neck, back of scalp, face, limb creases and backs of the wrists. In white children, the rash is most marked in the flexures: behind the knees, on the inside of the elbow joints, around the wrists, as well as the hands, ankles, neck and around the eyes. In black and Asian children, the rash is often on the extensor surface of the joints and may have a more follicular appearance.In adults, the neck, the backs of the hands, the groin, around the anus, the ankles and the feet are the most common sites. The rash of intertrigo is caused by a fungal infection and is found in skin folds or occluded areas such as under the breasts in women and in the groin or armpits.
Occupation/contact
Contact dermatitis may be caused by substances that irritate the skin or spark off an allergic reaction. Irritant contact dermatitis is most commonly caused by prolonged exposure to water (wet work). Typical occupations include cleaning, hairdressing, food processing, fishing and metal engineering. Substances that can irritate the skin include alkaline cleansing agents, degreasing agents, solvents and oils. Such substances either cause direct and rapid damage to the skin or, in the case of weaker irritants, exert their irritant effect after continued exposure. Napkin dermatitis is an example of irritant dermatitis, and can be complicated by infection, e.g. thrush. In other cases, the contact dermatitis is caused by an allergic re- sponse to substances which include chromates (present in cement and rust-preventive paint), nickel (present in costume jewellery and as plating on scissors), rubber and resins (two-part glues and the resin colophony in adhesive plasters), dyes, certain plants (e.g. primula), oxidising and reducing agents (as used by hairdressers when perming hair), and medications (including topical corticosteroids, lanolin, neo- mycin, cetyl stearyl alcohol). Eye make-up can also cause allergic contact dermatitis. Clues as to whether or not a contact problem is present can be gleaned from knowledge of site of rash, details of job and hobbies, onset of rash and agents handled, and improvement of rash when away from work or on holiday.Previous history
Patients may ask the pharmacist to recommend treatment for eczema, which has been diagnosed by the doctor. In cases of mild to moderate eczema, it would be reasonable for the pharmacist to recommend the use of emollients and to advise on skin care. Topical hydrocortisone and clobetasone preparations can be recommended for the treatment of mild to moderate eczema. However, where severe or infected exacerbations of eczema have occurred, the patient is best referred to the doctor. Occasionally, pharmacists receive requests for topical hydrocorti- sone or clobetasone products from patients on the recommendation oftheir doctors. It can be difficult to explain why such a sale cannot legally be made if the product is for use on the face or anogenital area or for severe eczema. Pharmacists can minimise such problems by ensuring that local family doctors (especially those in training) are aware of the restrictions that apply to the sale of hydrocortisone and clobetasone OTC.
History of hay fever/asthma Many eczema sufferers have associated hay fever and/or asthma. There is often a family history (in about 80% of cases) of eczema, hay fever or asthma. Eczema occurring in such situations is called atopic eczema. The pharmacist can enquire about the family history of these conditions.
Aggravating factors
Atopic eczema may be worsened during the hay fever season and by house dust or animal danders. Factors that dry the skin such as soaps or detergents and cold wind can aggravate the condition. Certain clothing such as woollen material can irritate the skin. In a small minority of sufferers (less than 5%), cow’s milk, eggs and food colouring (tartrazine) have been implicated. Emotional factors, stress and worry can sometimes exacerbate eczema. Antiseptic solutions applied directly to the skin or added to the bathwater can irritate the skin.
Medication
contact dermatitis may be caused or made worse by sensitisation to topical medicaments. The pharmacist should ask which treatments have already been used. Topically applied local anaesthetics, antihis- tamines, antibiotics and antiseptics can all provoke allergic dermatitis. Lanolin used to be a common sensitiser. Very highly purified lanolin is now available, and sensitisation problems appear to have been eradi- cated. Some preservatives may cause sensitisation. Information about different preparations and their formulations can be obtained from the local pharmacist or from the manufacturer of the product. The BNF is also a good source of information on this subject, with a list of additives for each topical product and excipients that may be associ- ated with sensitization. If the patient has used a preparation, which the pharmacist con- siders appropriate for the condition, correctly but there has been no improvement or the condition has worsened, the patient should see the doctor.
Treatment timescale
Most cases of mild to moderate atopic eczema, irritant and allergic dermatitis should respond to skin care and treatment with OTC products. If no improvement has been noted after 1 week, referral to the doctor is advisable.
Management
Skin rashes tend quite understandably to cause much anxiety. There is also a social stigma associated with skin disease. Many patients will therefore have been seen by their doctor. Pharmacists are most likely to be involved when the diagnosis has already been made or when the condition first presents but is very mild. However, with increasing recognition that patients can manage mild to moderate eczema, and as much of the management involves advice and the use of emollients, the pharmacist is in a good position to help, with short-term use of OTC topical steroids where needed. Where the pharmacist is able to identify a cause of irritant or allergic dermatitis, topical hydrocortisone or clobetasone may be recommended.
Emollients
Emollients are the key to managing eczema and are medically inert creams and ointments which can be used to soothe the skin, reduce irritation, prevent the skin from drying, act as a protective layer and be used as a soap substitute. They may be applied directly to the skin or added to the bathwater. There are many different types of emollient preparation that vary in their degree of greasiness. The greasy preparations such as white soft paraffin are often the most effective, especially with very dry skin, but have the disadvantage of being messy and unpleasant to use. Patient preference is very important and plays a major part in compliance with emollient treatments. Patients will understandably not use a preparation they find unacceptable. Patients may need to try several different emollients before they find one that suits them, and they may
need to have several different products (e.g. for use as a moisturiser, for use in the bath, for use as a soap substitute when washing or showering). Emollient preparations should be used as often as needed to keep the skin hydrated and moist. Several and frequent applications each day may be required to achieve this. Standard soaps have a drying effect on the skin and can make eczema worse. Aqueous cream can be used as a soap substitute. It should be applied to dry skin and rinsed off with water. Proprietary skin washes are also available. Adding emulsifying ointment or a proprietary bath oil to the bath is helpful. Emulsifying ointment should first be mixed with water (1 or 2 tablespoonfuls of ointment in a bowl of hot water) before being added to the bath to ensure distribution in the bathwater. Some patients with eczema believe, incorrectly, that bathing will make their eczema worse. This is not the case providing appropriate emollient products are used and stand- ard soaps and perfumed bath products are avoided, and in fact, bathing to remove skin debris and crusts is beneficial.
Advice This could include the identification of possible aggravating or pre- cipitating factors. If the history is suggestive of an occupationally associated contact dermatitis, then referral is advisable. The doctor may feel in turn that referral to a dermatologist is appropriate. It is sometimes necessary for a specialist to perform patch testing to iden- tify the cause of contact dermatitis. Further advice could be given regarding the use of ordinary soaps that tend to dry the skin and their alternatives (soap substitutes). If steroid creams have been prescribed and emollients are to be used, the pharmacist is in a good position to check that the patient understands the way in which they should be used.
Topical corticosteroids
Hydrocortisone cream and ointment and clobetasone 0.05% can be sold OTC for a limited range of indications. Topical hydrocortisone OTC is licensed for the treatment of irritant and allergic dermatitis, insect bites and mild to moderate eczema. OTC hydrocortisone is contraindicated where the skin is infected (e.g. athlete’s foot or cold sores), in acne, on the face and anogenital areas. Children aged over 10 and adults can be treated, and any course must not be longer than 1 week. Only proprietary OTC brands of topical hydrocortisone can be used; dispensing packs may not be sold. Topical clobetasone 0.05% is a P medicine for the short-term treat- ment and control of patches of eczema and dermatitis in people aged
12 and over. The indications include atopic eczema and primary irritant or allergic dermatitis and exclude seborrhoeic dermatitis
Antipruritics
Antipruritic preparations are sometimes useful although evidence of effectiveness is lacking. The itch of eczema is not histamine-related so the use of antihistamines other than that of sedation at night is not indicated. Aqueous calamine cream can be used and adding 1% menthol gives additional antipruritic and cooling actions. Crotamiton can reduce the discomfort of itchy skin and is avail- able in cream and lotion forms. A combination product containing crotamiton with hydrocortisone is available. Indications for use are the same as for topical hydrocortisone for contact dermatitis (irritant or allergic), insect bites or stings, and mild to moderate eczema. The same restrictions on use apply (see ‘Topical corticoster- oids’ above).
Support for patients The National Eczema Society provides information and support through its website www.eczema.org, a telephone helpline and written information.
Eczema and dermatitis in practice
Patients’ perspectives
‘I have lived with eczema all my life. I am now 33. My father had eczema and asthma. And the youngest of my three children also suffers with eczema. I know the heartache of this disease well. I have learned to control my eczema through my lifetime, but it takes quite a lot of trial and error to find the things that work and to avoid the things that set it off. Parents of kids with eczema need to listen to them and be patient with them because they are probably miserable, like I was as a child. ‘By the time I was about 18 or 19 my eczema had practically gone. My skin is still very sensitive and quite dry but is mostly OK. I go through phases where it breaks out behind my knees, on my forearms, on the back of my neck and on my lower back. When this happens, extra moisturiser and OTC hydrocortisone cream bring it under control again. ‘Managing atopic dermatitis is like taking care of the family car. When the car breaks down, you take it to the mechanic and get it fixed. That’s like managing a flare-up of eczema with topical
steroids...but the maintenance is still needed.Your car may be mended, but you still have to put oil in it regularly or the engine will seize up. And, like your car, you can do everything right – change the oil when you’re supposed to – and it can still break down on you.’


Comments
Post a Comment